What is runner's knee?
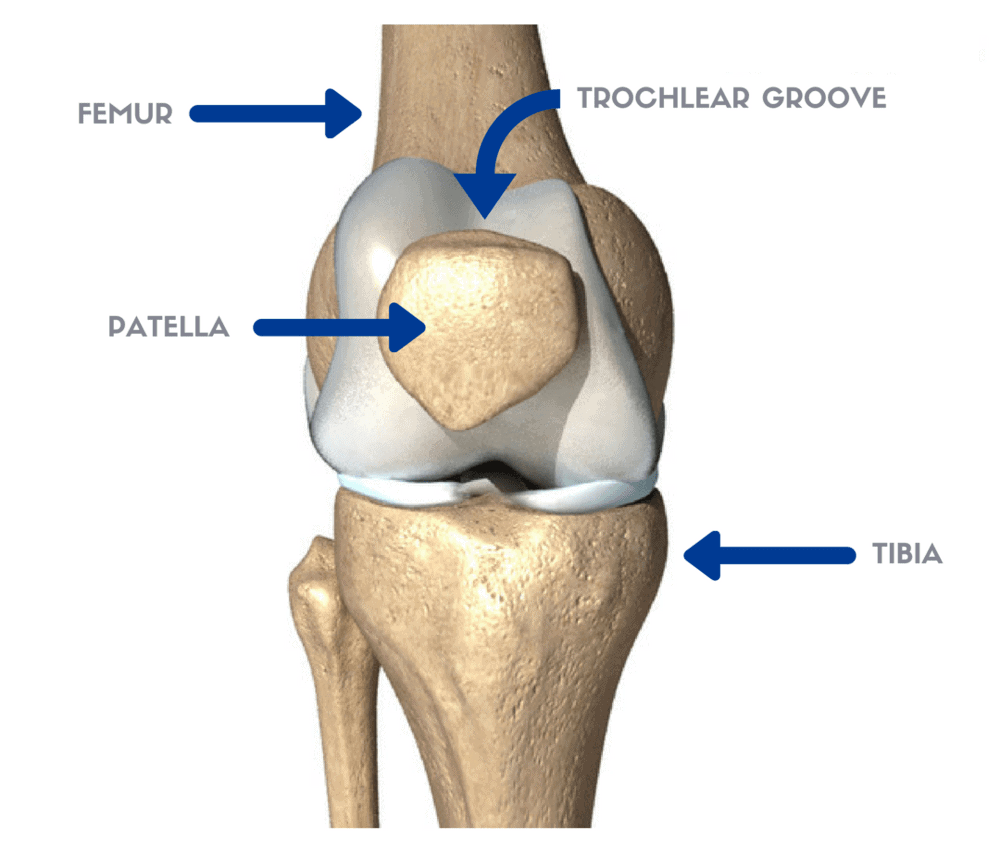
Runner's knee, also known as patellofemoral pain syndrome (PFPS) or chondromalacia patellae, is a common knee condition in adolescents, young adults and runners.1 It is characterized by pain around or behind the knee cap - known as the patella - that is usually difficult to localize to one specific spot. Due to the location at the front of the knee and the difficulty in determining if the patella is truly the source of symptoms, PFPS is sometimes given the broader label of anterior knee pain.2
Common symptoms of runner’s knee may include:
- Clicking or grinding noises in the knee (known as crepitus)
- Mild swelling
- Tenderness to touch around the kneecap
- Pain after prolonged sitting or transitioning from sitting to standing
- Aggravated by activities that load the knee (running, squatting, stair climbing and descent)
Patellofemoral pain syndrome is a clinical diagnosis, meaning that imaging studies such as x-ray or MRI scans are not typically needed. There are a variety of tests performed in the clinic that are used to detect patellofemoral pain such as the step down test:
Why do I have patellofemoral pain?
Runner’s knee starts gradually and is most commonly caused by excessive load on the patellofemoral joint. The patellofemoral joint is the articulation between the patella and the femur (i.e. the thigh bone and the knee cap). As the knee is flexed, there is more contact between the underside of the patella and the femur. At the same time, contact pressures increase during knee flexion. In the graph below, contact forces during various knee flexion angles for normal kneecap alignment is compared to a kneecap that sits higher (alta) or lower (infera) in the groove.3
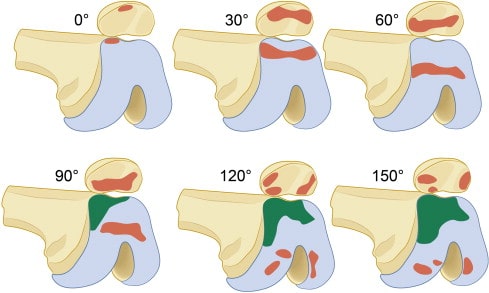
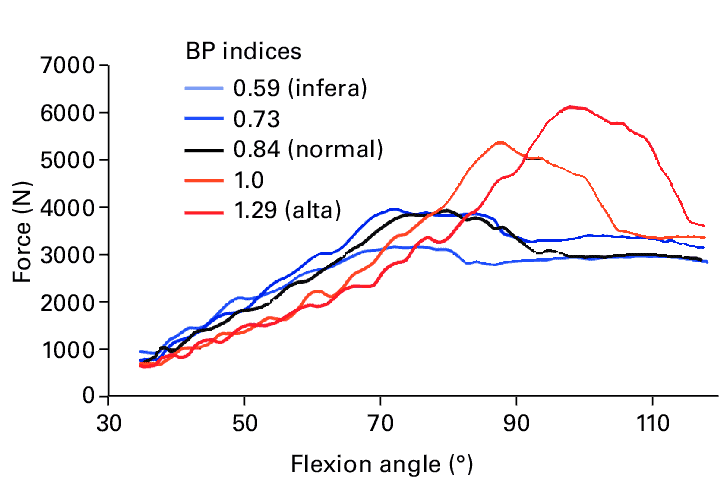
It is still unclear why patellofemoral pain develops, however there are three main theories.
Biomechanical factors
Movement patterns can influence the positioning of the knee and the tracking of the kneecap. Studies have shown that altered movements patterns are present in people with patellofemoral pain.4 These changes can include:
- Pelvis drop on the opposite hip (pulls the knee cap outwards)
- Hip internal rotation (changes the ‘groove’ where the knee cap moves within)
- Weak thigh muscles (the knee has difficulty absorbing the forces placed on it)
- Foot arch collapse (alters the tracking of the kneecap)
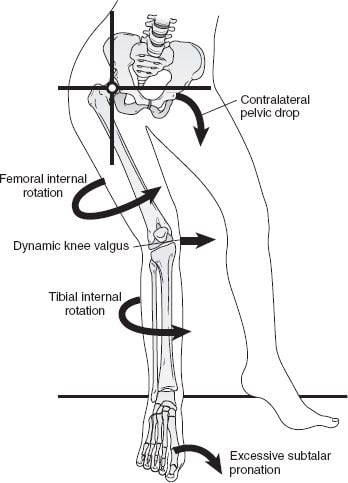
Not everyone will have these altered movement patterns. It is also difficult to detect these biomechanical factors with the naked eye. Research laboratories use marker-based camera systems to detect these changes, however it is time-consuming and impractical in a clinical setting. At Kinetic Labs, we use a markerless motion capture system to analyze movement biomechanics, allowing us to see subtle movement variabilities that often go unnoticed. In the video below, the patient has reduced knee flexion on the right leg when landing from a single leg jump.
Tissue homeostasis
As previously mentioned, increased load on the knee joint is often the main trigger for developing patellofemoral pain. This is a common occurrence in runners when increasing mileage during race training. Many people do “too much too soon”, which irritates the knee joint. It is important to gradually start or progress the intensity of activities to prevent onset of patellofemoral pain syndrome.5
Below is a side view of the knee taken during a bone scan. In a bone scan, a small amount of radioactive dye is used to detect areas of increased bone metabolism. The denser white areas in Figure A indicate a loss of homeostasis due to overloading of the patellofemoral joint. Figure B shows normal bone metabolism in the same knee 4 months later, after conservative treatment.2
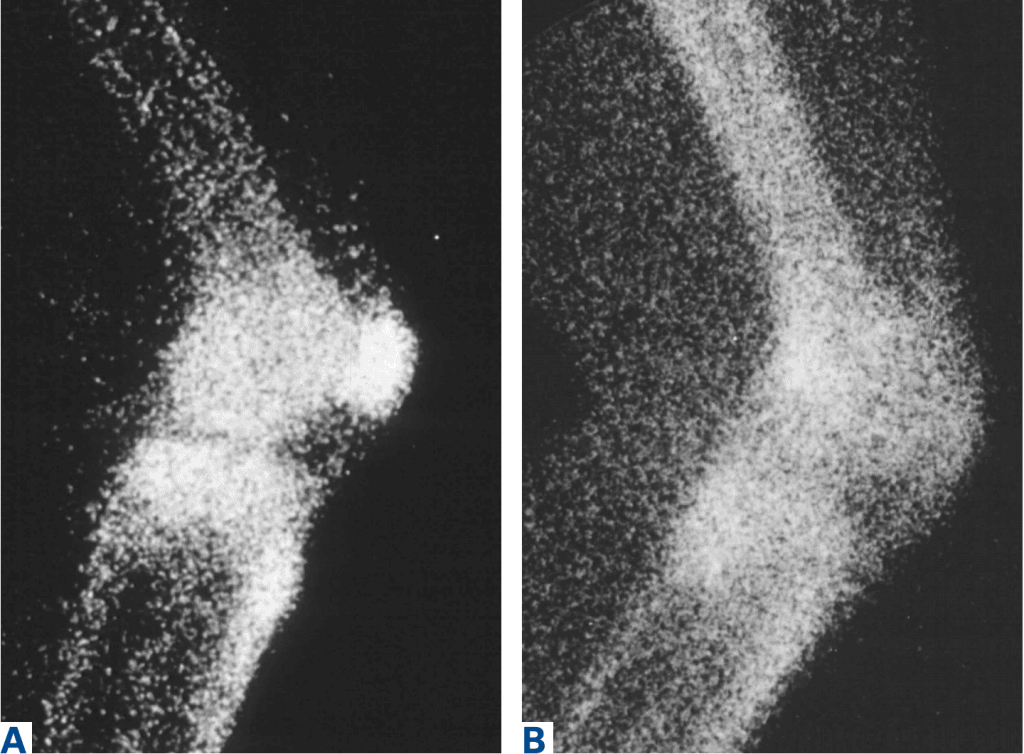
It takes many weeks for bone metabolism to return to normal. Therefore, it is important to not fall into a pattern of overloading the knee joint. Allowing the knee to settle down before gradually progressing the forces on it is one of the first goals of treatment.
Other factors
While the above two categories are usually the main drivers of anterior knee pain, other factors have been identified. Anxiety, depression, fear of movement and excessive worrying (known as catastrophizing) can play a role in keeping pain levels elevated, especially in cases of persistent patellofemoral pain. Sometimes it is not enough to address only the biomechanical and tissue factors. As in all musculoskeletal conditions, a comprehensive holistic approach is needed.
What is the best treatment for runner’s knee?
A treatment plan must address the main factors involved in your specific case in order to be successful. A well designed treatment plan contains the following elements:6
- Specific advice/education
- Progressive exercise program
- Movement retraining
- Load management
- Supportive modalities such as manual therapy, acupuncture, taping, and orthotics (as needed to reduce pain and facilitate exercise)
Do orthotics help with runner’s knee?
Orthotics can be useful for short term knee pain relief in some cases. Both prefabricated and custom orthotics can change the biomechanics at the ankle and help with pain reduction.7
Running shoe type can also reduce knee pain by lowering the forces at the knee. One study looked at minimalist shoes versus cushioned shoes in rearfoot strike runners and found reduced forces at knee when wearing minimalist shoes.8

What are the best exercises for runners knee?
A progressive exercise and movement retraining program is the most effective strategy for treating patellofemoral pain. Exercise improves tissue tolerance, allowing your knee to handle more load, as well as having analgesic effects.
Exercise should target the muscles of the lower leg including the hip, knee and ankle.9 Hip weakness is common in men and women with patellofemoral pain compared with healthy adults.10 Muscle strength testing can determine which areas to improve through exercise. You can self assess your hip and knee strength by following the tests below.
The gold standard for measuring muscle strength is a force dynamometer. This device can detect small changes in force produced by any muscle group. Unfortunately, most clinical settings don’t have access to this device and instead use less reliable methods such as manual muscle testing. At Kinetic Labs, we developed a force dynamometer that integrates with our software so that we can track trends in muscle strength over time.
Conclusion
Runner’s knee is usually self-limiting. The more load that is placed on the knee, the worse it feels. The exception to this is in individuals with persistent knee pain, where pain levels may not match changes in load.11 Increased load occurs with activities involving deep knee flexion, especially in weightbearing positions. Avoiding or reducing these activities is a good first step to allow the patellofemoral joint to settle down. Progressive strengthening combined with other interventions is an effective recovery strategy.
References
- https://link.springer.com/chapter/10.1007/978-3-319-52567-9_74
- https://pubmed.ncbi.nlm.nih.gov/28437494/
- https://pubmed.ncbi.nlm.nih.gov/19258610/
- https://www.ncbi.nlm.nih.gov/pubmed/29109118
- https://www.ncbi.nlm.nih.gov/pubmed/15995427
- https://www.jospt.org/doi/full/10.2519/jospt.2019.0302#_i126
- https://www.sciencedirect.com/science/article/abs/pii/S0966636219317813
- https://www.mdpi.com/2076-3417/9/19/4176
- https://pubmed.ncbi.nlm.nih.gov/24175148/
- https://bjsm.bmj.com/content/48/14/1088.abstract?sid=b7ff354e-631f-4592-802c-6acbbbf68160
- https://journals.sagepub.com/doi/abs/10.1177/0363546519889623



.png)
