Optimization.
It’s all about improvement, efficiency and becoming the best you can be. As an athlete, this is always the goal. At Kinetic Labs, we have the same goal. How can we reduce injury risk? Improve treatment outcomes? Understand more about how our athletes move?
Motion capture offers a solution. Using state of the art technology, the process of quantifying human movement is streamlined and simplified. Our system captures useful information for athletes about their movement patterns with acceptable levels of validity and reliability1-5. Our system is markerless; allowing for a fast setup and reliable tracking between sessions and testers. 3D analysis takes the guesswork out of the clinical evaluation of movement. Instead it captures movement patterns that can be too quick or subtle to detect with the naked eye and 2D cameras. At Kinetic Labs, we provide a complete data driven report on your specific movement biomechanics. This report will be used to assess potential for injury risk, performance measures and general motion health.
How did we get here?
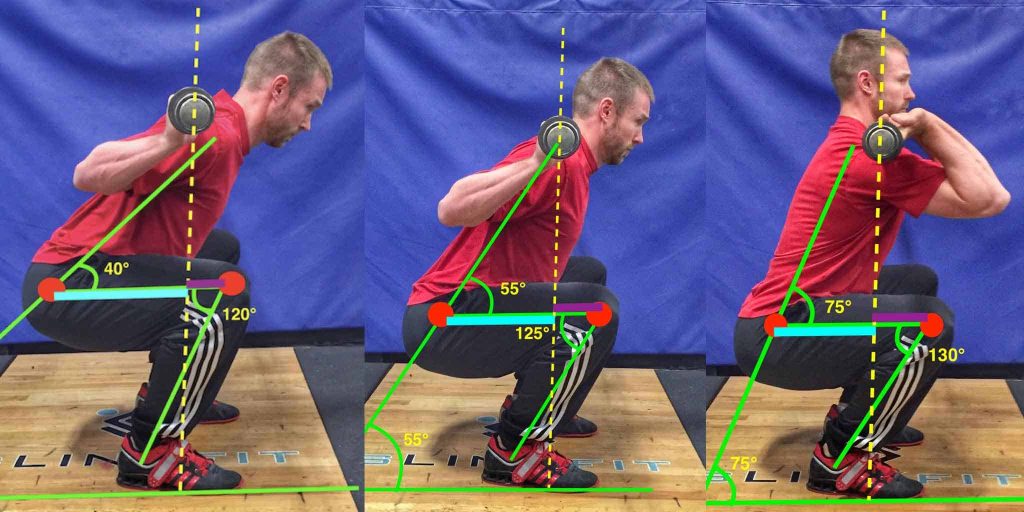
The use of optical sensors in movement therapy has become more common in clinical practice. Many practices use 2D video applications in order to quantify human movement. This system is considered to be feasible and practical for clinical use. At its beginning, still images were taken of the athlete and lines were drawn by the tester to measure joint angles. Now, it is possible to track using marker based automatic tracking as well as markerless methods. Movement about three axes can be difficult to interpret using 2D video, especially for more dynamic and complex motion6-8. Regardless, this method is still superior in comparison to observation with the naked eye, as it combats the issues of self-report and recall error.
Through the use of multiple synchronized cameras, 3D motion capture is able to record human movement from every angle. While measuring 3D kinematics, we are concerned with the motion of the body and how the body is moving with regard to position, speed and acceleration in 3D space. The most common technique of 3D motion capture is a passive optical motion capture system. This uses retroreflective markers that are affixed to specific areas of the body, which are tracked by infrared cameras. This method is not unlike the behind the scenes work that is done to create characters in film like Gollum in Lord of the Rings or the Pandorian Na’vi from AVATAR. Marker based 3D motion capture is regarded as the gold standard of motion analysis9. These systems are classified as research grade and provide valid and reliable data for human kinematics. However, the time required to place the markers, set up the system, clean and process the data is inefficient for use in a clinical setting; bringing us to the latest in this technology.

Markerless motion capture provides a resolution for clinicians who want the practicality of 2D analysis and the accuracy of 3D marker-based systems. This method substantially reduces athlete preparation time compared to marker-based systems, as there are no markers to be attached to the skin. This also removes the potential for inconsistency of marker placement between sessions and testers5. The athlete is free to move as naturally as possible as there is no potential for marker interference. Data cleaning and post processing time for the clinician are also greatly reduced, allowing for the athlete to receive their results almost immediately.
Here’s where it gets techy. Skip ahead if you wish.
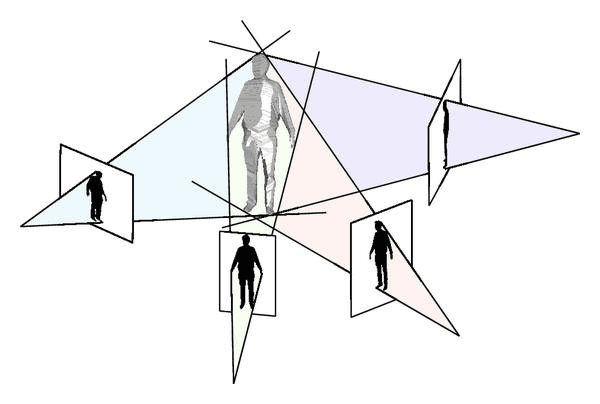
At Kinetic Labs, we use an 8-camera passive vision system to measure human movement. A passive system is one that works by capturing images as opposed to light information (i.e. infrared), which is ideal for capturing athletes in their natural environment10. Our system uses a visual hull reconstruction and background subtraction method in order to create the 3D representation of the athlete within the motion capture volume. The visual hull of the subject is the approximation of the volume occupied by the athlete. Each instant in time captured by the camera system constructs one visual hull for the athlete. Each of the eight cameras projects the subject’s silhouette back to the 3D volume, and the intersection of these projections generates the athlete’s visual hull5. This visual hull is detected from the difference between the current frame and the background image, which is a representation of the motion capture volume without the athlete in it11. A specific template skeleton is then fitted into the visual hull and transformed, using an automatic scaling process, into a subject specific skeleton4. This consists of multiple 3D Gauss functions to estimate joint center positions and local optimization using a deep learning algorithm to refine the silhouettes12. This entire process takes seconds to complete.
Using 3D motion capture allows our clinicians to monitor continuous physiological movement of their athletes. Through this technology, we are not limited to seeing and measuring just one part of an athlete’s functional movement. Data for postures, body position and multiple joints are available simultaneously for the entirety of the range of motion for almost any type of movement. Motions are recorded for review or further investigation with minimal bias. This is especially valuable during dynamic movement, which often happens too quickly to analyze in real time. If the athlete is performing a squat, instead of reporting on what may have looked like some good form from the angle of view, we can now consider the combined action at the ankle, knee, hip, trunk and displacement of centre of mass, visible from any angle. Once captured, data will be uploaded and analyzed, and a report will be created showing the unique musculoskeletal movement signature of the athlete.

So, how can you benefit from this?
Injury Risk Prevention and Rehabilitation
Our priority is reducing the risk of injury to our athletes. We want to keep you playing your sport as long as possible. We can’t stop you from getting hit by an offensive tackle, but we can try and minimize the risk factors associated with non-contact injuries. Non-contact injuries are those which occur without a direct blow to the joint, and account for 70-95% of all sports injuries13-18. Failure of the tissue in a non-contact situation happens when the strength capacity of the structure is exceeded by the demand or stress placed upon it. By screening for kinematic risk factors which have been associated with injury occurrence, we can begin to identify potentially hazardous patterns and address them proactively.

If you are actively recovering from injury, our goal is to help you return to your peak physical fitness and help to avoid re-injury. We can track your rehabilitation progress while simultaneously checking for movement inefficiencies. By monitoring your recovery over time, we can compare and report on changes in how your musculoskeletal system is working together during movement, and where imbalances exist which may place stress on your body. Understanding your motion profile is a valuable aspect of your treatment and prevention plan. Gaining awareness and perspective about how you move will help you progress toward your specific goals and take control of your health. These reports can be shared with coaches, trainers, physiotherapists, and other health professionals to ensure a cohesive understanding of your strengths and weaknesses from your entire support team as you prepare to return to play.
Performance Measures
Whether you want to jump higher, run faster or get stronger, we are here to help you understand how you move and how to get there from a musculoskeletal standpoint. We want to go faster too, and our system allows us to do that by tracking your movement in real-time, allowing us to gain insights almost immediately. Using markerless 3D motion capture is time-effective and minimizes the potential for human error or bias. We can produce analytics and performance measures to consider range of motion, how you are producing force, symmetries, and asymmetries. Reports can be generated for you, your coach or your physical trainer instantly in order to gain a deeper perspective of your movement. This will allow them to create more custom and effective training protocols to enable you to achieve optimal athletic performance and a competitive edge. By continuing to monitor movement over time, the effectiveness of your training regimen can be evaluated. If you are a developing athlete, physical maturity can be monitored to be proactive about musculoskeletal health. In this way, our assessment can help you achieve marginal gains and gross movement efficiency, ultimately contributing to your success as an athlete.
Movement Health
Is everything looking okay? Our Performance Analysis provides you with exactly that — a baseline. This is a look at your starting point to guide your everyday movement health goals, whatever they may be. Whether your goal is to maintain strength or become more mobile, our analysis gives you feedback in real-time to give you insights into where you currently stand. Naturally, as we age, our mobility, strength, and balance decrease19-22, and these changes can be subtle. Considering a baseline movement analysis as a routine checkup allows us to note these changes over time and provide you with insights to help you achieve your best quality of life.
References
- Corazza, S., Mündermann, L., Chaudhari, A.M., Demattio, T., Cobelli, C. & Andriacchi, T.P. (2006). A Markerless Motion Capture System to Study Musculoskeletal Biomechanics: Visual Hull and Simulated Annealing Approach. Biomedical Engineering 34(6), 1019-1029.
- Harsted, S., Holsgaard-Larsen, A., Hestbæk, L., Boyle, E. & Lauridsen, H.H. (2019). Concurrent validity of lower extremity kinematics and jump characteristics captured in pre-school children by a markerless 3D motion capture system. Chiropractic & Manual Therapies 27(39).
- Harsted, S., Kawchuk, G., Guan, R., Skallgård, T., Hesby, B.B., Boyle, E. & Kjaer, P. (2019). c. Poster session presented at WFC Biannual Congress / ECU Convention 2019, Berlin, Germany.
- Perrott, M.A., Pizzari, T., Cook, J. & McClelland, J.A. (2017). Comparison of lower limb and trunk kinematics between markerless and marker-based motion capture systems. Gait & Posture 52, 57-61
- Sandau, M., Koblauch, H., Moeslind, T.B., Anæs, H., Alkjær, T. & Simonsen, E.B. (2014) Markerless motion capture can provide reliable 3D gait kinematics in the sagittal and frontal plane. Medical Engineering & Physics 36, 1168-1175.
- Englander et al. (2019). A Comparison of Knee Abduction Angles Measured by a 3D Anatomic Coordinate System Versus Videographic Analysis: Implications for Anterior Cruciate Ligament Injury. Orthopaedic Journal of Sports Medicine 7(1), 1-7.
- Mousavi et al. (2020). Validity and reliability of a smartphone motion analysis app for lower limb kinematics during treadmill running. Physical Therapy in Sport 43, 27-35.
- Neal et al. (2020). Is markerless, smart phone recorded two-dimensional video a clinically useful measure of relevant lower limb kinematics in runners with patellofemoral pain? A validity and reliability study. Physical Therapy in Sport 43, 36-42.
- Schurr SA, Marshall AN, Resch JE, Saliba SA. (2017). Two-Dimensional Video Analysis Is Comparable To 3D Motion Capture In Lower Extremity Movement Assessment. The International Journal of Sports Physical Therapy 12(2), 163-172.
- Alahmari, A., Herrington, L., Jones R. (2020). Concurrent validity of two-dimensional video analysis of lower-extremity frontal plane of movement during multidirectional single-leg landing. Physical Therapy in Sport 42, 40-45.
- Mackey, A.H., Walt, S.E., Lobb, G.A. & Stott, N.S. (2005) Reliability of upper and lower limb three-dimensional kinematics in children with hemiplegia. Gait & Posture 22, 1-9.
- Mündermann, L., Corazza, S. & Andriacchi, T.P. (2006). The evolution of methods for the capture of human movement leading to markerless motion capture for biomechanical applications. Journal of NeuroEngineering and Rehabilitation 3(6).
- Piccardi, M. (2004). Background subtraction techniques: a review. IEEE International Conference on Systems, Man and Cybernetics 4, 3099-3104.
- Stoll, C., Hasler, N., Gall, J., Seidel, H. & Theobalt, C. (2011). Fast Articulated Motion Tracking using a Sums of Gaussians Body Model. IEEE International Conference on Computer Vision 2011, 951-958.
- Bisciotti, G.N., Chamari, K., Cena, E., Bisciotti, A., Corsini, A. & Volpi, P. (2019). Anterior cruciate ligament injury risk factors in football. The Journal of Sports Medicine and Physical Fitness 59(10), 1724-1738.
- Ekstrand, J., Hägglund, M. & Walden, M. (2011). Epidemiology of Muscle Injuries in Professional Football (Soccer). The American Journal of Sports Medicine 39(6), 1226-1232.
- Langdon, E., Snodgrass, S.J., Young, J.L., Miller, A. & Callister, R. (2019) Posture of rugby league players and its relationship to non-contact lower limb injury: A prospective cohort study. Physical Therapy in Sport 40, 27-32.
- Lee, J.W., Mok, K., Chan, H.C., Yung, P.S. & Chan, K. (2014). A prospective epidemiological study of injury incidence and injury patterns in a Hong Kong male professional football league during the competitive season. Asia-Pacific Journal of Sports Medicine, Arthroscopy, Rehabilitation and Technology 1, 119-125.
- Lu, D., McCall, A., Jones, M., Kovalchik, S., Steinweg, J., Gelis, L. & Duffield, R. (2020). Injury epidemiology in Australian male professional soccer. Journal of Science and Medicine in Sport.
- Reis, G.F., Santos, T.R.T., Lasmar, R.C.P., Júnior, O.O., Lopes, R.F.F., Foncesca, S.T. (2015). Sports injuries profile of a first division Brazilian soccer team: a descriptive cohort study. Brazilian Journal of Physical Therapy 19(5), 390-397.
- Daly, R.M., Rosengren, B.E., Alwis, G. Ahlborg, H.G., Sernbo, I. & Karlsson, M.K. (2013). Gender specific age-related changes in bone density, muscle strength and functional performance in the elderly: a-10-year prospective population-based study. BMC Geriatrics 13(71).
- Guralnik, J.M., Ferrucci, L., Simonsick, E.M., Salive, M.E. & Wallace, R.B. (1995). Lower-Extremity Function in Persons over the Age of 70 Years as a Predictor of Subsequent Disability. The New England Journal of Medicine 332, 556-562
- King, G.W., Abreu, E.L., Kelly, P.J. & Brotto, M. (2019) Neural control of postural sway: Relationship to strength measures in young and elderly adults. Experimental Gerontology 118, 39-44.
- Spartano et al. (2019). Objective physical activity and physical performance in middle-aged and older adults. Experimental Gerontology 119, 203-211.


.png)